Published March 25, 2024
Building a Career in Mental Health Care: Nursing Alum Jonathan Campos

Jonathan Campos believes mental health care should be easily accessible to all. “At any moment of anyone’s life, something could happen that could majorly affect their mental health,” says the 2023 graduate of the NYU Rory Meyers College of Nursing.
But the issue wasn’t always on his radar. Like many students Jonathan didn’t know what he wanted to study in college. A volunteering opportunity working with patients with dementia after high school illuminated his career path. “I learned about compassion and empathy working with those patients,” he says. “When that program ended, I realized I wanted to be in health care, specifically nursing, because there’s more patient interaction.”
The Road to NYU
Jonathan initially enrolled in a community college in upstate New York. However, he was interested in NYU because of its vast resources and facilities, plus the opportunity to pursue a minor in Childhood and Adolescent Mental Health Studies. Eventually, he transferred and, like all NYU nursing students, was thrown into the deep end from the beginning. “In the first semester, we worked directly with nurses,” he says. “By the second semester, we were doing everything: starting catheters, giving medications. From that point on, it was very hands-on.”

Experiential Learning
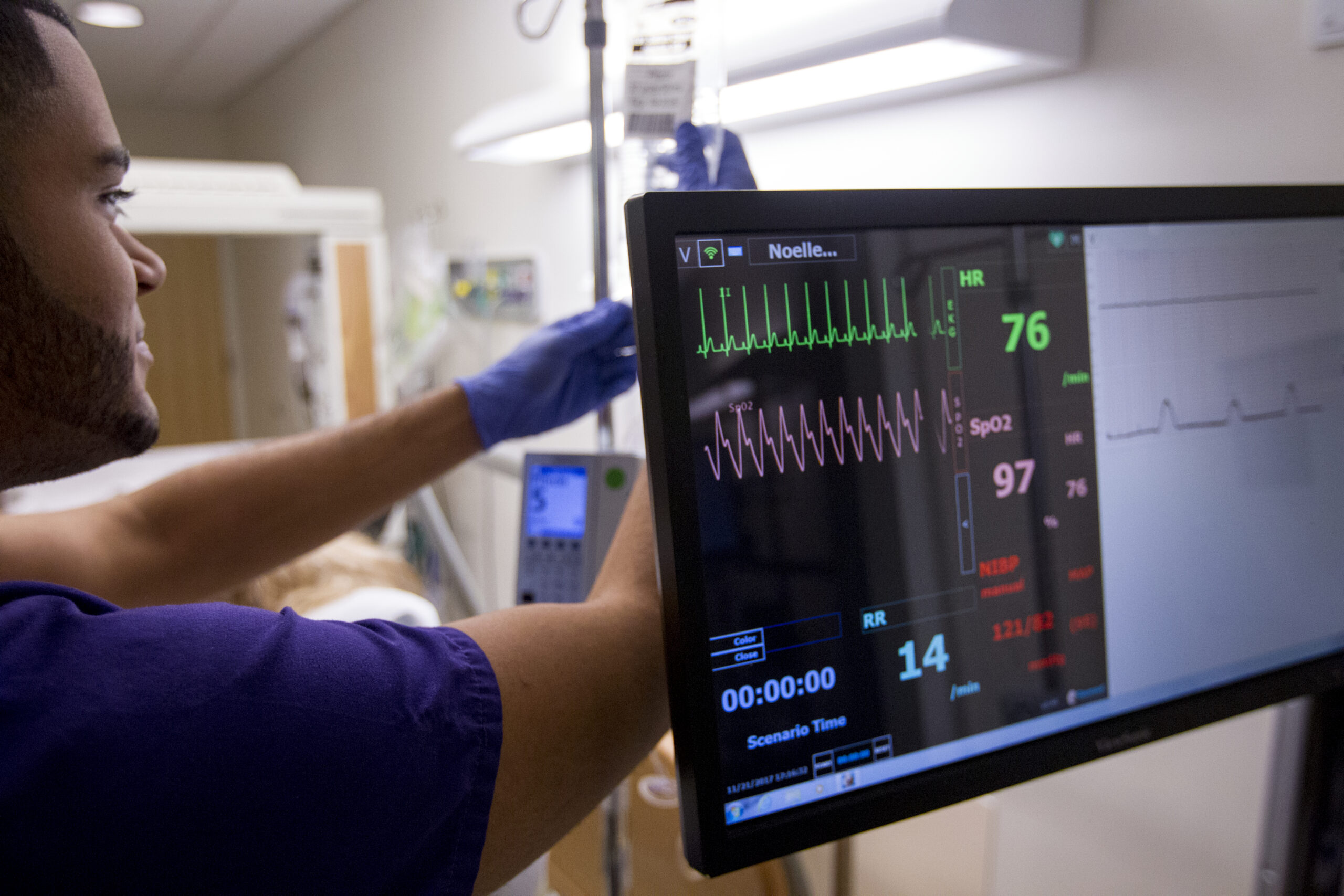
NYU students work directly with registered nurses and patients in some of the most advanced health-care facilities in the country. But they also have access to the state-of-the-art Clinical Simulation Learning Center. The learning center is a 10,000-square-foot space where nursing students can hone their skills. Students have access to computerized mannequins, task trainers, and other high-tech hospital equipment in this space. Plus, they learn in a program fully committed to treating diverse patient populations with the utmost sensitivity and respect. In fact, these practices are critical for proper physical and mental health care. “I think NYU just does a superb job at inclusivity,” Jonathan says. “How to treat people of different ethnic backgrounds or people who identify as all different genders. I haven’t really experienced that from other nursing programs,” he says.

An International Fellowship Opportunity
After Jonathan graduated in the spring of 2023, he immediately set off to Italy for a six-week fellowship with Doctors in Italy. The program places nursing and medical students in Italian cities where they shadow medical professionals in a clinical setting. “It was a great opportunity to rotate and see different specialties,” Jonathan says. “I could tailor my training to say, ‘I did a day in this particular specialty, but I didn’t really like it. Can we do a different one today?’ And they would accommodate.”
What’s more, the program has no language requirement. Participants work four days a week, spend one day on structured tours of their city and surrounding areas, and have two additional days off to explore independently. While Jonathan learned about Italian culture and Florence (his assigned location) on the weekend, his clinical rotations exposed him to critical cultural differences. He realized that the communal aspect of care led to better physical and mental health outcomes. “The importance of community was a big takeaway,” he says. “In each patient room, there were four patient beds, and they were all concerned about each other’s health. They would try to care for one another and create a sense of community with people they didn’t know. It made me realize how important creating a community and being involved in patient care can be instrumental to recovery.”
The Next Step
When Jonathan returned home, he plunged into another program in the specialty that initially brought him to nursing school: mental health care. He’s now enrolled in a master’s degree program at Duke University to become a psychiatric nurse practitioner, which will allow him to work with patients as a therapist and prescribe medications if needed. As he works to complete his degree, he hopes to help patients, wherever they are, access care when they need it most. “Telehealth allows for more communities with lower access to health care to obtain the psychiatric help that they need for mental health,” he says. “Now a lot of practitioners are moving toward telehealth for practicing therapy or even reviewing medication. That is something more I’m leaning toward, too, based on this big need that exists in psychiatric health.”



